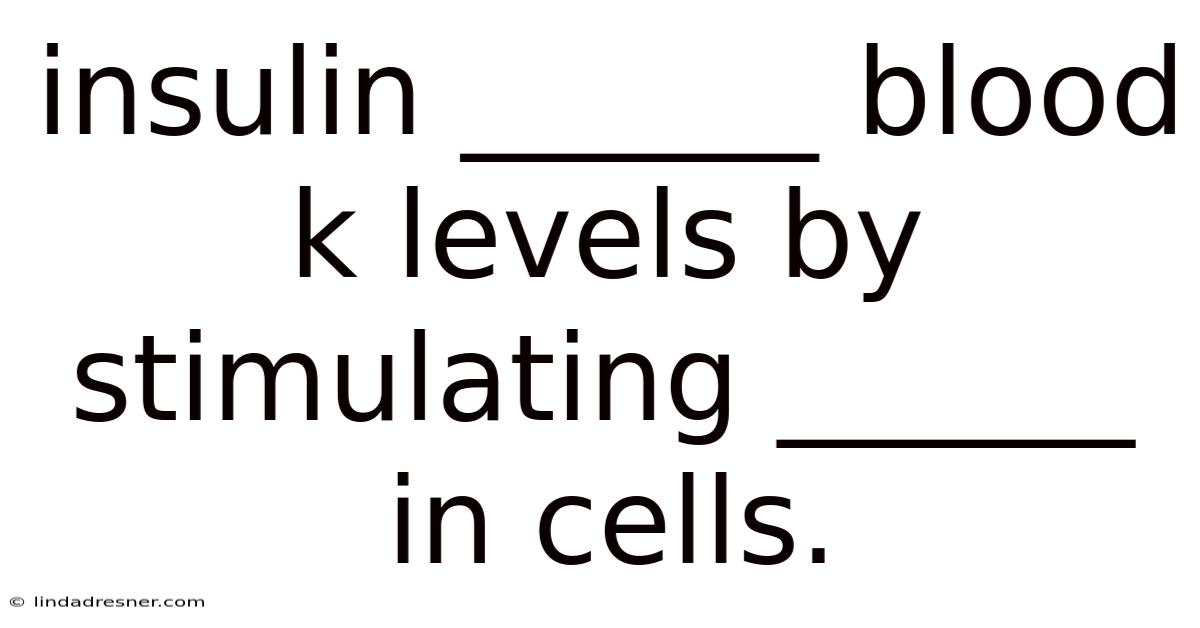Insulin acts as the body's primary regulator for lowering elevated blood glucose levels by triggering the uptake of glucose into cells. This essential hormone, produced by the beta cells in the pancreas, orchestrates a complex signaling cascade that facilitates glucose transport across cellular membranes, primarily in muscle, fat, and liver tissue. Understanding this process is crucial for managing conditions like diabetes and appreciating how the body maintains metabolic balance Easy to understand, harder to ignore..
How Insulin Works: The Glucose Uptake Mechanism
The process begins when blood glucose levels rise, such as after a meal. In response, the pancreas releases insulin into the bloodstream. Insulin then binds to specific receptors on the surface of target cells, particularly muscle and adipose (fat) cells. This binding event is the critical first step, initiating a cascade of intracellular signals Took long enough..
The Key Players: GLUT4 Transporters
The primary mechanism for glucose entry into most cells relies on specialized proteins called glucose transporter proteins. Worth adding: the most significant of these for insulin-responsive tissues is GLUT4. And unlike some other glucose transporters (like GLUT1 in the brain), GLUT4 is not constantly embedded in the cell membrane. Instead, it resides in intracellular storage vesicles Not complicated — just consistent. Still holds up..
Stimulating Glucose Uptake: The Insulin Signal Cascade
When insulin binds to its receptor on the cell surface, it triggers a series of events inside the cell:
- Receptor Activation: Insulin binding causes a conformational change in the receptor, activating its intrinsic tyrosine kinase activity. This enzyme phosphorylates itself and specific insulin receptor substrates (IRS proteins) nearby.
- Signal Amplification: Phosphorylated IRS proteins act as docking stations, recruiting and activating downstream signaling molecules like PI3K (Phosphoinositide 3-Kinase). PI3K converts phosphatidylinositol 4,5-bisphosphate (PIP2) into phosphatidylinositol 3,4,5-trisphosphate (PIP3).
- GLUT4 Mobilization: PIP3 acts as a second messenger, recruiting proteins like Akt (Protein Kinase B) to the inner surface of the cell membrane. Akt, in turn, phosphorylates and activates key proteins involved in GLUT4 trafficking.
- Vesicle Fusion: The activated signaling proteins cause the intracellular vesicles containing GLUT4 transporters to move to the cell membrane and fuse with it. This fusion inserts the GLUT4 transporters into the membrane.
- Glucose Entry: With GLUT4 transporters now embedded in the membrane, glucose molecules in the bloodstream can diffuse down their concentration gradient through these channels into the cell. This process is facilitated diffusion, not active transport.
The Net Effect: Lowering Blood Glucose
This orchestrated movement of GLUT4 transporters to the cell surface dramatically increases the number of glucose channels available on the cell membrane. As these cells absorb glucose from the blood, the overall concentration of glucose in the bloodstream decreases. This means glucose uptake into muscle and fat cells accelerates significantly. This is the fundamental mechanism by which insulin effectively lowers elevated blood glucose levels after a meal, restoring the body to a state of metabolic homeostasis.
Scientific Explanation: The Insulin Signaling Pathway
The pathway described above is a highly conserved insulin signaling cascade. It involves complex phosphorylation events and the activation of numerous downstream effectors. Key components include:
- Insulin Receptor (IR): A receptor tyrosine kinase (RTK).
- Insulin Receptor Substrates (IRS): Adaptor proteins phosphorylated by the IR.
- PI3K (Phosphoinositide 3-Kinase): Phosphorylates PIP2 to PIP3.
- PIP3 (Phosphatidylinositol 3,4,5-trisphosphate): A second messenger.
- PDK1 (Phosphoinositide-Dependent Kinase 1) & Akt (Protein Kinase B): Downstream kinases activated by PIP3.
- GSK3β (Glycogen Synthase Kinase 3 Beta): Phosphorylated and inactivated by Akt, allowing glycogen synthase activation.
- AS160 (TBC1D4): A Rab GTPase-activating protein (GAP) for Rab proteins involved in vesicle trafficking. Akt phosphorylates AS160, inhibiting its GAP activity and allowing Rab proteins to activate vesicle fusion machinery (like SNARE proteins).
- Rab Proteins (e.g., Rab10, Rab11): Small GTPases regulating vesicle trafficking.
- Vesicle Trafficking Machinery: Including motor proteins (kinesin, dynein) and fusion proteins (SNAREs).
This pathway is not only vital for glucose uptake but also regulates other metabolic processes like glycogen synthesis, lipid synthesis, and protein synthesis, all of which contribute to lowering blood glucose levels and storing energy.
Frequently Asked Questions (FAQ)
- Q: What happens if insulin signaling is impaired? A: Insulin resistance or deficiency leads to hyperglycemia (high blood sugar), the hallmark of type 2 and type 1 diabetes. Cells fail to take up glucose effectively, causing it to build up in the blood.
- Q: Can cells take up glucose without insulin? A: Yes, some cells (like brain cells and red blood cells) can use GLUT1 transporters that are constitutively active and don't require insulin. Still, insulin is essential for the rapid and regulated uptake of glucose into muscle and fat cells.
- Q: How does the liver respond to insulin? A: Insulin promotes glycogen synthesis and inhibits glycogen breakdown in the liver. It also stimulates glycolysis and fatty acid synthesis. While liver cells (hepatocytes) don't primarily use GLUT4 for glucose uptake, insulin regulates the enzymes involved in glucose metabolism within the liver itself.
- Q: What is the role of exercise in glucose uptake? A: Exercise increases the translocation of GLUT4 transporters to the muscle cell membrane independently of insulin. This is a crucial mechanism for lowering blood glucose during and after physical activity.
- Q: Are there other hormones that affect blood glucose? A: Absolutely. Glucagon, released by pancreatic alpha cells when blood sugar is low, stimulates glycogen breakdown and gluconeogenesis in the liver to raise blood glucose. Epinephrine, cortisol, and growth hormone also play roles in counter-regulatory glucose release during stress or fasting.
Conclusion
Insulin is a master regulator of glucose homeostasis. Its ability to stimulate glucose uptake into muscle and fat cells by mobilizing and inserting GLUT4 transporters into the cell membrane is a cornerstone of this regulation. This detailed signaling cascade, involving receptor binding, second messengers like PIP3, and the precise control
Continuing naturally from the provided text:
Vesicle Trafficking & Metabolic Integration: The PIP3-dependent activation of Rab proteins (like Rab10 and Rab11) orchestrates the precise delivery of GLUT4-containing vesicles to the plasma membrane. This process, involving motor proteins (kinesin, dynein) transporting vesicles along microtubules and the fusion machinery (SNARE proteins) facilitating membrane merger, is exquisitely timed and regulated. Beyond glucose uptake, this pathway is a central hub for metabolic coordination. Insulin signaling, amplified by PIP3, simultaneously stimulates pathways leading to glycogen synthesis in the liver and muscle, activates lipogenesis in adipose tissue, and promotes protein synthesis in muscle. This integrated response ensures surplus glucose is efficiently stored as glycogen or converted to triglycerides, while anabolic processes are upregulated to support cellular growth and energy reserves. Because of this, insulin's actions lower blood glucose levels acutely and promote long-term energy storage and utilization efficiency.
The Consequences of Dysregulation: When this finely tuned system falters, as in insulin resistance or deficiency, the consequences are profound. Impaired GLUT4 translocation and vesicle trafficking reduce glucose uptake capacity, forcing the pancreas to secrete more insulin (hyperinsulinemia) to compensate. Over time, this compensatory mechanism exhausts pancreatic beta cells, leading to relative insulin deficiency (type 2 diabetes) or absolute deficiency (type 1 diabetes). The resulting hyperglycemia has systemic effects: chronic high blood sugar damages blood vessels (contributing to cardiovascular disease), nerves (neuropathy), kidneys (nephropathy), and eyes (retinopathy), while disrupting lipid metabolism and protein synthesis pathways. The liver, no longer responsive to insulin's inhibitory signals, continues glycogenolysis and gluconeogenesis unabated, further elevating blood glucose Turns out it matters..
Conclusion: Insulin is the quintessential hormone of metabolic homeostasis, acting through a sophisticated signaling cascade initiated by receptor tyrosine kinase activation and amplified by second messengers like PIP3. This cascade precisely controls the trafficking and fusion of GLUT4-containing vesicles, enabling rapid and regulated glucose uptake into insulin-sensitive tissues like muscle and fat. Crucially, this pathway extends far beyond glucose transport, integrating with and stimulating key anabolic processes – glycogen synthesis, lipogenesis, and protein synthesis – that collectively lower blood glucose and store energy. The disruption of this nuanced system, whether through cellular resistance to insulin's signals or failure of insulin production, is the fundamental defect underlying diabetes mellitus and its devastating complications. Understanding the molecular mechanisms of insulin signaling, particularly the critical role of vesicle trafficking and fusion machinery, remains essential for developing targeted therapies to restore metabolic balance and mitigate the global burden of insulin-resistant diseases Most people skip this — try not to..